Chronic Hepatitis B: Practical Guide to Care, Testing & Treatment
More than 250 million people live with chronic hepatitis B (HBV) worldwide — and many can live long, healthy lives if the infection is diagnosed and managed. If you or someone you care about has HBV, this page gives clear, useful steps: how doctors test for it, when treatment helps, what medicines work, and everyday choices that protect your liver and others.
What causes chronic hepatitis B and how it's diagnosed
HBV is a virus spread through blood and some body fluids. Common ways it moves are from mother to baby at birth, through shared needles, or unprotected sex. A short acute infection becomes chronic when the virus stays in the body for more than six months.
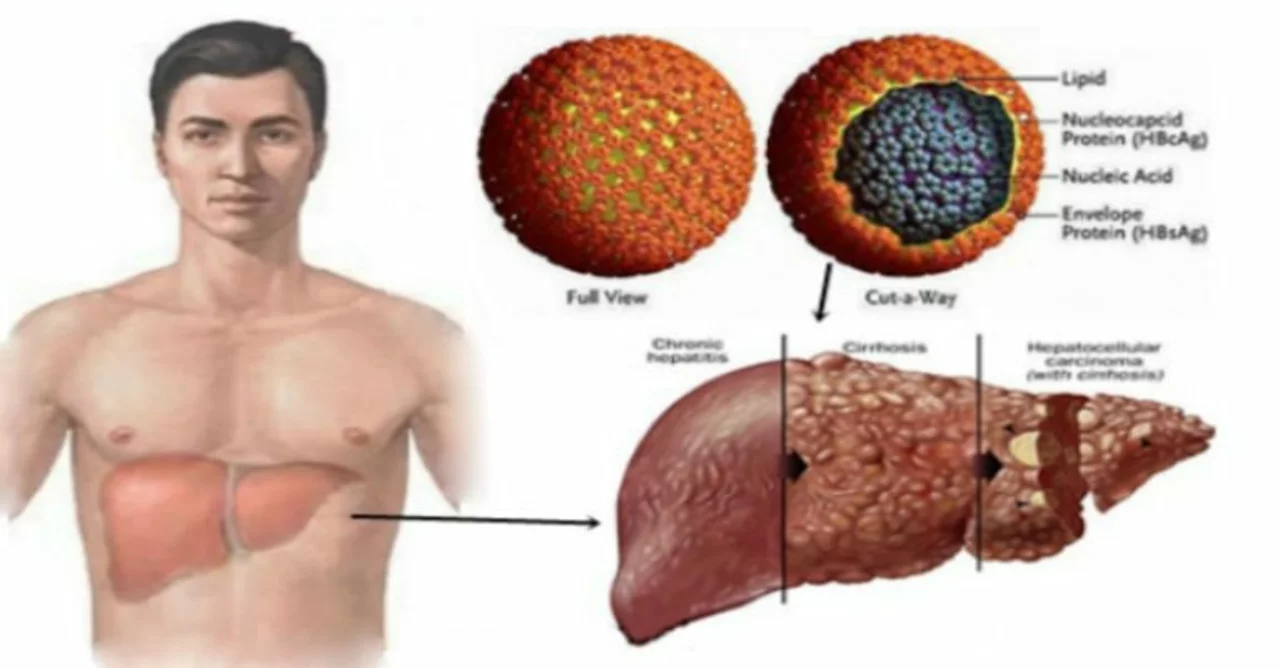
Tests doctors use: HBsAg (surface antigen) to confirm chronic infection, HBV DNA to measure how much virus is in the blood, HBeAg to check infectivity, and liver enzymes (ALT/AST) to see liver inflammation. Imaging or a FibroScan helps check scarring (fibrosis). If you have a positive HBsAg, ask for HBV DNA and ALT to know the next steps.
Treatment, monitoring, and living with HBV
Treatment aims to stop liver damage and lower the risk of cirrhosis and liver cancer. First-line antiviral medicines are tenofovir (TDF or TAF) and entecavir — they reduce viral load and are safe for long-term use for most people. Not everyone needs immediate treatment: doctors usually start meds when HBV DNA is high, ALT is elevated, or there is evidence of liver damage.
Monitoring matters. If you’re not on treatment, expect HBV DNA and ALT checks every 3–6 months at first, then spacing out if stable. People with cirrhosis or high cancer risk should have a liver ultrasound every 6 months to screen for hepatocellular carcinoma (HCC).
Pregnancy needs special attention. Pregnant people with high viral loads often start tenofovir in the third trimester to reduce transmission risk to the baby. Newborns should receive the hepatitis B vaccine and HBV immune globulin at birth when the parent is positive.
Protect others: tell close contacts so they can get tested and vaccinated if needed. Avoid sharing needles, razors, or toothbrushes. Use condoms if needed until you know your partner’s status.
Simple lifestyle steps help the liver: avoid alcohol or keep it very low, manage weight and blood sugar, get vaccinated against hepatitis A, and treat other health issues like obesity and diabetes. Stay in care — regular visits mean problems get caught early.
If you need help finding a specialist or affordable meds, ask your primary doctor, local health clinic, or patient support groups. With the right testing, monitoring, and treatment, chronic hepatitis B can be managed — and you can keep living well.
Chronic Hepatitis B and the Elderly: What You Need to Know
As a blogger, I feel it's essential to spread awareness about chronic Hepatitis B, especially in the elderly population. This viral infection affects the liver and can lead to severe health complications if left untreated. It's crucial for our elderly loved ones to get screened and vaccinated, as their immune systems may be weaker, making it harder for them to fight off infections. Additionally, proper care and management of the condition can help prevent the progression of the disease and improve their quality of life. Let's join hands to protect our seniors and keep them healthy by spreading awareness about chronic Hepatitis B.
View More