Subarachnoid hemorrhage: how to spot it fast and what to do
That sudden, brutal headache people describe as "the worst of my life" is the red flag for a subarachnoid hemorrhage (SAH). It usually comes on without warning and often means a blood vessel on the brain surface has burst. If you feel this kind of headache, think and act fast—SAH is an emergency where minutes matter.
So what exactly causes it? The most common reason is a ruptured aneurysm — a weak spot in an artery that balloons and then leaks or breaks. Less often, trauma, certain blood disorders, or high blood pressure can cause bleeding into the space between the brain and its covering (the subarachnoid space).
Quick checklist: signs and immediate steps
Watch for these symptoms: sudden severe headache, neck stiffness, nausea or vomiting, light sensitivity, brief loss of consciousness, or new confusion and weakness. If someone has any of these after a sudden headache, call emergency services right away. Do not drive them yourself unless there’s no alternative.
While waiting for help: keep the person still and calm, have them lie down with the head slightly elevated, and avoid painkillers that could mask symptoms unless directed by emergency staff. Don’t give aspirin or other blood thinners unless a doctor tells you to—those can make bleeding worse.
How doctors confirm SAH and what happens next
At the hospital, a non-contrast CT scan is the first test. It finds most cases quickly. If CT doesn’t show bleeding but suspicion remains high, doctors do a lumbar puncture (spinal tap) to check the cerebrospinal fluid for blood. After confirmation, they use angiography (CT, MR, or catheter angiogram) to find the bleeding source, often an aneurysm.
Treatment focuses on stopping the bleed and preventing complications. Two main procedures fix ruptured aneurysms: surgical clipping (open surgery) or endovascular coiling (inserting coils via a catheter). Which one the team chooses depends on aneurysm shape, size, and location, plus the patient’s condition.
Preventing and managing complications is just as important. Vasospasm—narrowing of brain arteries days after the bleed—can cause delayed strokes. Doctors monitor closely and use medications like nimodipine and sometimes interventions to keep blood flowing. Other issues include hydrocephalus (fluid buildup) and seizures; both need fast treatment.
Recovery varies. Some people recover well with timely care. Others face longer rehab for speech, movement, or cognitive problems. Follow-up imaging and blood pressure control, quitting smoking, and managing cholesterol lower the risk of another event.
If you suspect SAH, don’t second-guess it. Rapid recognition and immediate medical care are the best chance to limit damage and save a life.
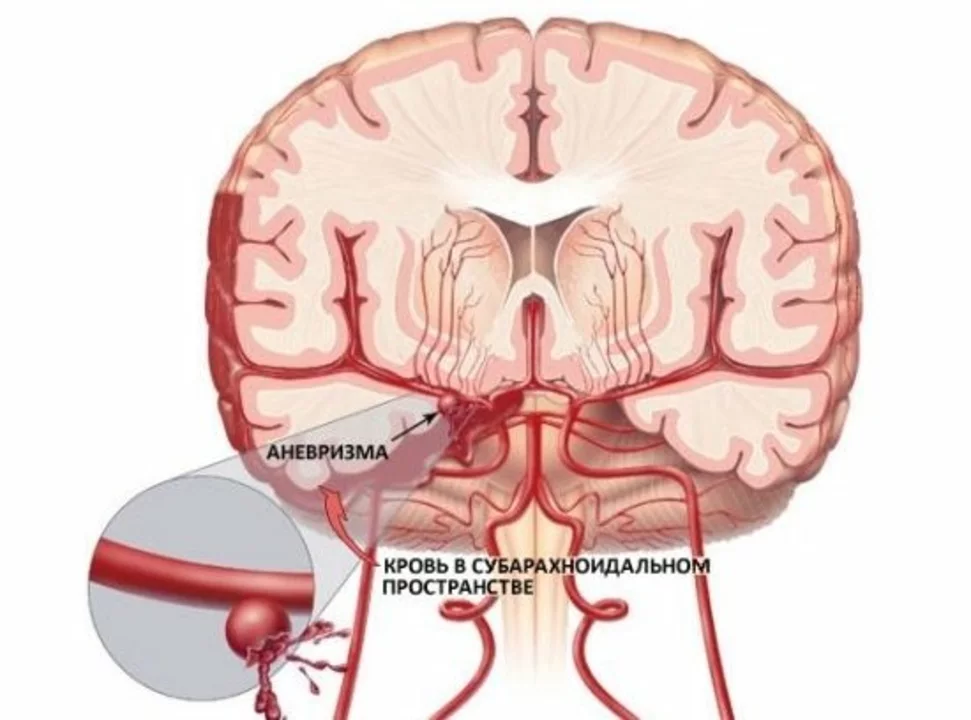
The Connection between Subarachnoid Hemorrhage and Aneurysms: A Closer Look
In my recent deep dive into the world of medical research, I've discovered an intriguing connection between subarachnoid hemorrhage and aneurysms. It turns out that a subarachnoid hemorrhage, which is a life-threatening type of stroke, often occurs when a brain aneurysm ruptures. This rupture can cause blood to leak into the space surrounding the brain, leading to severe complications. Interestingly, not all aneurysms pose a threat - only when they rupture does the risk of a subarachnoid hemorrhage increase. It's essential to be aware of this connection and take preventative measures, such as regular medical check-ups, to minimize the risk of experiencing either of these dangerous medical conditions.
View More